What if the very thing that makes a dangerous bacterium so hard to kill also turns out to be its greatest vulnerability? That is exactly the possibility scientists are now exploring — and early results suggest it could reshape how medicine fights some of the deadliest infections on the planet.
Researchers have identified a potential Achilles’ heel in antibiotic-resistant bacteria: a unique sugar molecule found exclusively on the outer surface of bacterial cells. According to recent research conducted in mice, targeting this molecule can expose the bacteria to the immune system, which then moves in to destroy the germs and clear the infection.
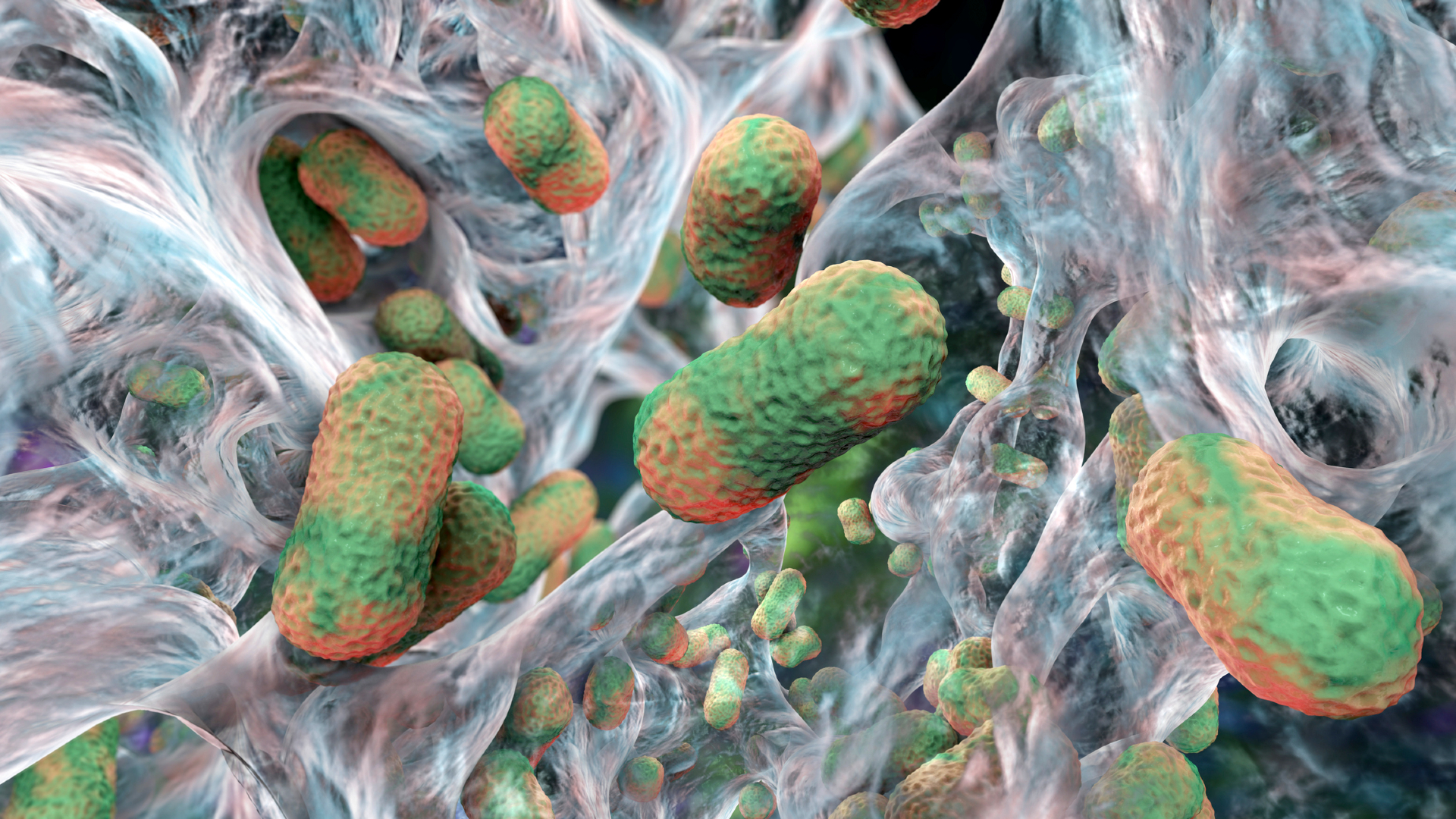
The discovery is particularly relevant to bacteria like Acinetobacter baumannii, a pathogen notorious for causing serious infections in hospital settings and for its ability to resist multiple classes of antibiotics. If this approach holds up in further testing, it could open a new front in the fight against superbugs — one that works with the body’s own defenses rather than relying solely on drugs the bacteria have learned to defeat.
Why Antibiotic-Resistant Bacteria Are Such a Serious Threat
Antibiotic resistance is not a distant or theoretical problem. It is already killing people. Bacteria evolve rapidly, and decades of antibiotic use — in medicine, agriculture, and elsewhere — have accelerated the development of strains that no longer respond to the drugs designed to stop them.
Acinetobacter baumannii is one of the most feared examples. It thrives in hospital environments, can survive on surfaces for extended periods, and has developed resistance to nearly every antibiotic currently available. Patients with weakened immune systems — those recovering from surgery, receiving cancer treatment, or in intensive care — are especially vulnerable.
The broader challenge is that developing new antibiotics is slow, expensive, and increasingly difficult. Bacteria can develop resistance to a new drug within years of its introduction. That reality has pushed researchers to look for entirely different strategies — and the sugar molecule discovery represents exactly that kind of lateral thinking.
The Science Behind the Weakness Researchers Found
The key to this potential breakthrough lies in a sugar molecule that appears only on the outside of bacterial cells — not on human cells. That distinction matters enormously, because it means any treatment designed to target this molecule would theoretically attack the bacteria without harming the patient’s own tissues.
The research, conducted in mice, showed that when this surface molecule is targeted, the bacteria become vulnerable to the immune system. Rather than hiding from the body’s natural defenses — which is part of how these pathogens cause such persistent and dangerous infections — the bacteria are effectively unmasked. The immune system can then identify and destroy them.
This approach is fundamentally different from traditional antibiotics, which typically work by directly killing bacteria or stopping them from reproducing. Instead, this strategy essentially strips away a layer of protection the bacteria use to evade detection.
What the Research Has — and Has Not — Confirmed Yet
It is worth being clear about where the science currently stands. The findings so far come from studies in mice, which is a critical early step but not the same as a proven treatment for humans. The path from a promising mouse study to a safe and effective human therapy is long and involves multiple phases of testing.
| Aspect | Current Status |
|---|---|
| Target identified | Confirmed — unique sugar molecule on bacterial cell surface |
| Tested in mice | Yes — immune system cleared infection when molecule was targeted |
| Tested in humans | Not yet confirmed |
| Bacteria studied | Includes Acinetobacter baumannii and other antibiotic-resistant strains |
| Mechanism | Exposing bacteria to immune system by targeting surface molecule |
| Treatment availability | Not yet — further research required |
Researchers still need to demonstrate that the same effect can be replicated in humans. That process will involve safety testing, efficacy trials, and regulatory review — a timeline that typically spans years, not months.
Why This Approach Could Matter Beyond One Bacteria
One of the more significant aspects of this discovery is that it may not be limited to a single type of bacteria. The research appears to apply to antibiotic-resistant bacteria more broadly, not just Acinetobacter baumannii — though that pathogen is among the most prominent examples studied.
If the sugar molecule exists across multiple strains of drug-resistant bacteria, a treatment targeting it could potentially work against a range of superbugs. That would be a meaningful development given how fragmented the current landscape of treatments is — different antibiotics for different bacteria, with resistance emerging constantly.
Researchers and public health experts have long argued that the world needs not just new antibiotics but entirely new classes of approaches. Strategies that recruit the immune system rather than relying on chemical agents alone represent one such direction, and this research adds to that growing body of work.
What Comes Next for This Research
The immediate priority for scientists will be confirming whether the same mechanism that worked in mice also functions in human biology. The immune systems of mice and humans share many features but also differ in important ways, and results do not always transfer cleanly from one to the other.
Should human studies prove promising, the next stages would involve determining how best to deliver a treatment targeting the sugar molecule, assessing safety, and establishing what types of infections it could most effectively address.
For now, the discovery represents a genuine scientific lead — a potential crack in the armor of bacteria that have so far proven extraordinarily difficult to defeat. In a field that has struggled to keep pace with evolving pathogens, that is meaningful progress, even if a usable treatment remains some way off.
Frequently Asked Questions
What is the Achilles’ heel scientists discovered in antibiotic-resistant bacteria?
Researchers identified a unique sugar molecule found only on the outer surface of bacterial cells. Targeting this molecule appears to make bacteria vulnerable to the immune system.
Has this been tested in humans yet?
Not yet. The research demonstrating this effect has so far been conducted in mice. Whether the same results can be achieved in humans has not yet been confirmed.
What bacteria does this research focus on?
The research includes Acinetobacter baumannii, a drug-resistant bacterium commonly associated with hospital infections, as well as other antibiotic-resistant bacteria more broadly.
How is this different from regular antibiotics?
Rather than directly killing bacteria, this approach targets a surface molecule that allows the body’s own immune system to detect and destroy the bacteria — a fundamentally different mechanism.
When could a treatment based on this discovery become available?
This has not yet been confirmed. Moving from animal studies to an approved human treatment typically takes many years of additional testing and regulatory review.
Why does this discovery matter for people who get hospital infections?
Bacteria like Acinetobacter baumannii are extremely difficult to treat with existing antibiotics. A new approach that bypasses antibiotic resistance entirely could eventually offer options where few currently exist.





Leave a Reply