The very chemicals hospitals use to keep patients safe may be quietly helping dangerous bacteria become harder to kill — and early research suggests those bacteria could be traveling through the air to reach patients who never came near the original source.
A new early-stage study has raised a troubling possibility: a common antiseptic used to clean hospital patients’ skin can linger on surfaces for hours after application, and that lingering residue may be creating conditions where bacteria develop tolerance to the chemicals designed to eliminate them. The findings, while preliminary, point to a potential gap in hospital infection control that researchers are only beginning to understand.
For anyone who has ever been admitted to a hospital — or has a loved one in an intensive care unit — this is the kind of story that deserves close attention.
What “Antiseptic Tolerance” Actually Means
There’s an important distinction worth understanding here, because the language around bacterial resistance can get confusing fast.
When bacteria develop tolerance to an antiseptic, they become better at surviving certain concentrations of that chemical — more so than their non-tolerant peers. But they can still be killed by the standard doses used in clinical settings. This is different from full-blown resistance, where a bacteria can survive even the doses meant to destroy it.
Think of it on a sliding scale. A tolerant bacterium is harder to kill than a normal one, but it isn’t invincible. A resistant bacterium, however, may be almost impossible to eliminate with conventional treatments. The worry with tolerance is that it can be a stepping stone — a biological rehearsal — for something far more dangerous down the road.
Hospitals already face a serious and ongoing battle against antibiotic-resistant infections. The emergence of antiseptic-tolerant bacteria adds a new layer to that problem, one that targets the very first line of chemical defense used in clinical environments.
How Hospital Antiseptics May Be Backfiring
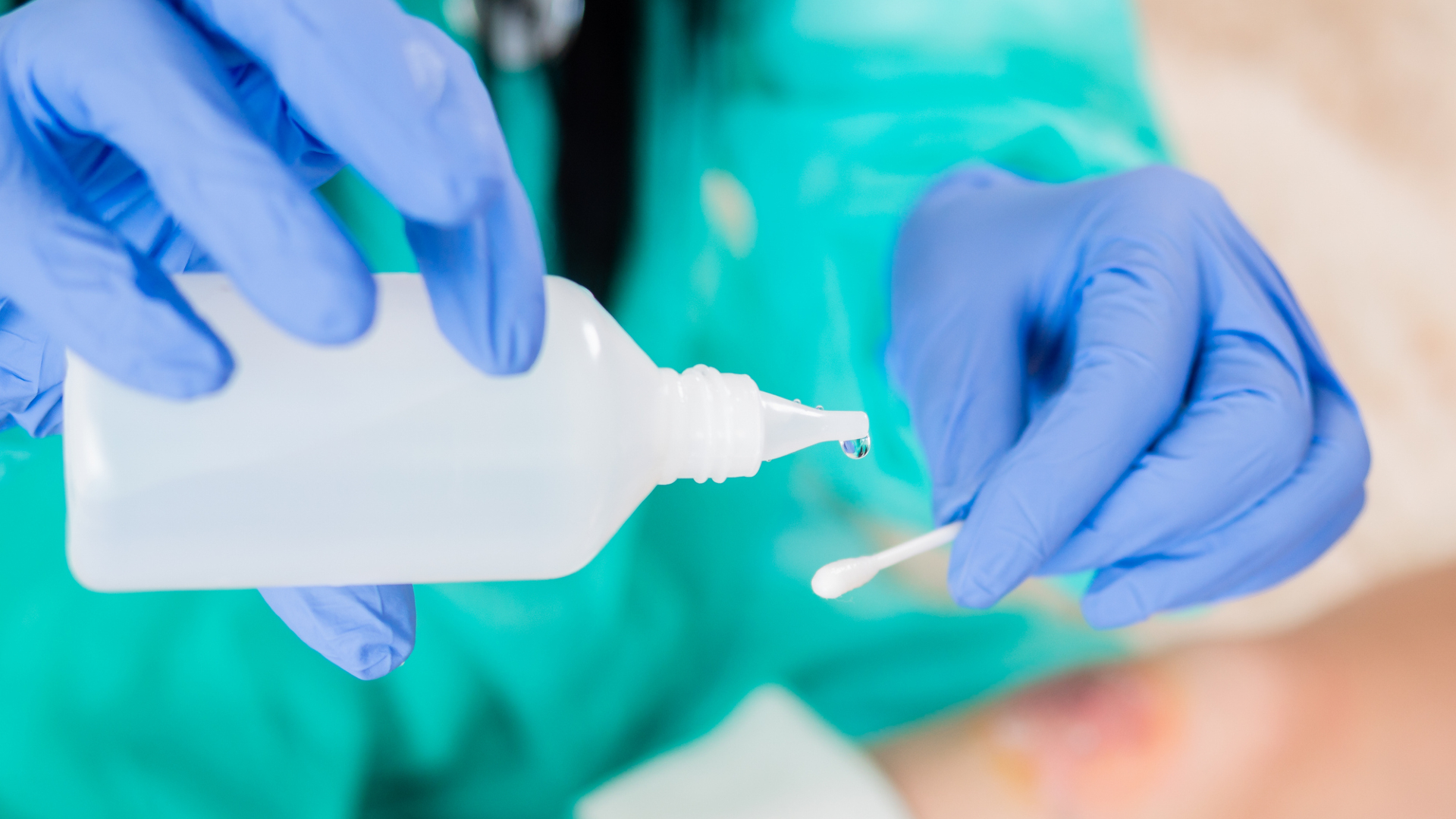
The antiseptic at the center of this early research is commonly used to clean patients’ skin before procedures — a routine step meant to reduce the risk of infection. According to the study, this chemical can persist on surfaces in ICU rooms for hours after it’s applied.
That prolonged presence on surfaces is the key concern. Rather than doing its job and disappearing, the antiseptic appears to linger at concentrations that may be enough to stress bacteria without fully eliminating them. That kind of low-level chemical pressure is exactly the type of environment that can push bacteria toward developing tolerance.
What makes this finding especially striking is the airborne dimension. The early research hints that antiseptic-tolerant bacteria may not stay put on the surfaces where they developed that tolerance. Instead, they may be spreading through the air within hospital rooms — potentially reaching patients who had no direct contact with the contaminated surface at all.
That airborne spread, if confirmed in further studies, would significantly complicate how hospitals approach infection prevention in enclosed ward environments like ICUs.
What the Early Evidence Suggests — And What It Doesn’t
It’s worth being clear about the limitations of what’s currently known. This is early-stage research. The findings are described as hints rather than confirmed conclusions, and the science will need to be replicated and expanded before hospitals would be expected to change their protocols based on this alone.
| Aspect of the Finding | Current Status |
|---|---|
| Antiseptic lingers on surfaces for hours | Indicated by early study |
| Surface residue encourages bacterial tolerance | Suggested by early research |
| Tolerant bacteria spread through hospital air | Early study hints at this — not yet confirmed |
| Tolerance leading to full antibiotic resistance | Not established by this research |
| Immediate risk to current hospital patients | Not confirmed — further study needed |
The distinction between tolerance and resistance matters here too. The bacteria identified in this context can still be killed by appropriate doses of antiseptics. The concern is more about the trajectory — whether environments that breed tolerance are inadvertently setting the stage for something worse over time.
Why ICU Patients Face the Highest Stakes
Intensive care units are where the sickest patients in a hospital are treated. They’re also environments where antiseptics are used heavily and frequently — precisely because the patients there are so vulnerable to infection. That combination makes the ICU both the most likely place for this kind of antiseptic residue to accumulate and the place where the consequences of bacterial tolerance would be most severe.
Patients in ICUs often have compromised immune systems, open wounds, surgical sites, or invasive devices like catheters and ventilators that create direct pathways for bacteria to enter the body. For these patients, even a bacterium that is merely tolerant — not fully resistant — could pose a meaningful threat if it reaches the wrong place in sufficient numbers.
The possibility that tolerant bacteria could travel through the air within these rooms raises questions about whether current ventilation, cleaning, and antiseptic application practices are fully accounting for this kind of indirect spread.
What Researchers and Hospitals May Need to Consider Next
Because this is early research, the immediate next step is further investigation. Scientists will need to study whether the airborne spread of antiseptic-tolerant bacteria is a consistent and reproducible finding, how far such bacteria can travel through hospital air, and whether tolerant strains are actually causing infections in patients.
Researchers and public health experts are likely to examine whether changes to how antiseptics are applied — including concentration, frequency, and surface coverage — could reduce the amount of residue left behind in clinical environments.
There may also be questions raised about hospital ventilation systems and whether air filtration in ICUs is adequate to intercept bacteria that become airborne. These are not simple or cheap problems to solve, which is part of why confirming the scale of the issue through further research is the essential first step.
For now, hospitals are not expected to change their antiseptic protocols based on this single preliminary study. But the research adds to a growing body of concern about how the environments designed to protect patients may, under certain conditions, be contributing to the evolution of harder-to-kill bacteria.
Frequently Asked Questions
What antiseptic is involved in this research?
The study involves a common antiseptic used in hospitals to clean patients’ skin before procedures. The specific product has not been named in the available source material.
Does this mean hospital antiseptics are no longer effective?
Not based on current evidence. Bacteria described as “tolerant” can still be killed by standard doses of antiseptics — they are simply harder to eliminate than normal bacteria at certain concentrations.
Can antiseptic-tolerant bacteria spread through the air?
Early research hints that this may be possible within ICU rooms, but this finding has not yet been confirmed and will require further study.
Is this the same as antibiotic resistance?
No. Antiseptic tolerance and antibiotic resistance are different things. Tolerance means bacteria survive some concentrations of a chemical more easily — it does not mean they are immune to standard clinical doses.
Should patients be worried about going to the hospital?
This is preliminary research and does not indicate an immediate or confirmed threat to hospital patients. Current antiseptic protocols remain in use and are not being changed based on this early study.
What happens next with this research?
Further studies will be needed to confirm whether antiseptic-tolerant bacteria reliably spread through hospital air and whether they pose a measurable risk to patients in ICUs and other clinical settings.





Leave a Reply